By Abbey Bigler
BU News Service
BOSTON – An elderly diabetic patient shuffles into a small doctor’s office in Montana for a checkup after traveling for nearly an hour. This particular woman and doctor’s office are fictional, but such distance from a physician is not uncommon in rural areas, where general practitioners are scarce and specialists are almost non-existent.
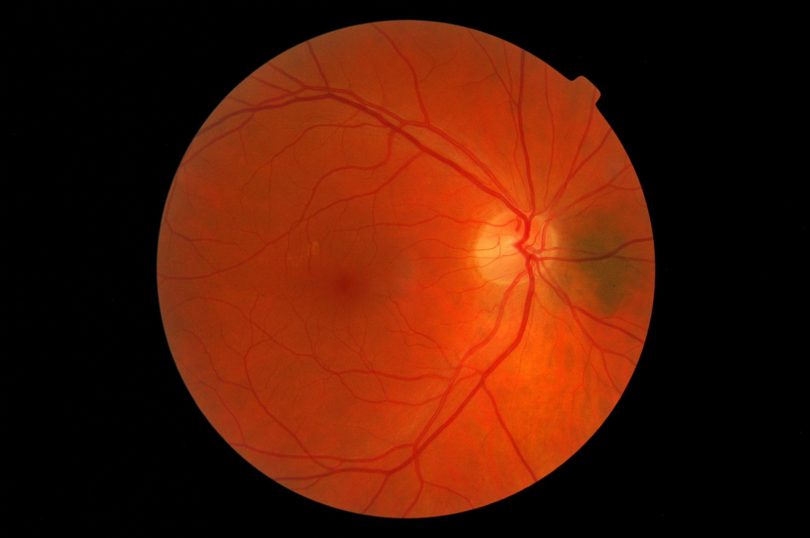
During the checkup, the doctor wants to screen the patient for diabetic retinopathy, a complication of diabetes in which the blood vessels at the back of the eyes become damaged. In the early stages, diabetic retinopathy may cause no symptoms or mild vision changes, but left untreated, it can lead to blindness.
Checking for diabetic retinopathy normally requires a visit to an eye specialist who will dilate a patient’s pupils to examine them. But that’s not necessary here: the doctor asks the woman to sit in front of a large white machine with a chin rest on one side and a touchscreen on the other, similar to the machines that shoot startling puffs of air into your eyes during an eye exam.
Rather than do that, this apparatus takes photos of the woman’s retinas. The doctor then pushes a button and within seconds receives a message from an artificial intelligence (AI) program that has processed the photos: “Negative for more than mild diabetic retinopathy; rescreen in 12 months,” the message says. The doctor completes the physical exam and sends the woman on her way, assured that she is still in good health.
Such a scenario could take place in the not-too-distant future. The disease-screening AI program described, called IDx-DR, received approval from the Food and Drug Administration (FDA) in April 2018. It is already being used in clinical settings and is far from the only AI technology you will find aiding medical diagnoses that require image analysis.
Until now, providing a second opinion has been the typical role of AI technologies that review medical images. The IDx-DR is the first AI approved by the FDA to provide a screening recommendation without a physician’s review. In short, it is the first AI empowered to act as a diagnostician.
Image-reviewing artificial intelligence used in medicine, sometimes referred to as computer-aided diagnosis, represents a small subset of AI research. Artificial intelligence is a huge and complex area of research that uses computers to mimic functions of a brain, such as sorting objects into categories. When these programs were first created, programmers trained them to screen images through machine learning, a process in which a program is given images and taught through computer code to identify an object.
For example, a programmer could tell an AI through
In 2012, an advance in AI, called deep learning, enabled researchers to train AI programs more efficiently. Now, instead of telling an AI what characteristics to look for through code, researchers give the AI a huge set of images and tell it that each image falls into one of two categories: “disease condition” or “normal.” The AI then looks for similarities among the images in each category, developing its own definitions of the categories. To test the AI program after training it, researchers give it other images that they know show diseased or healthy systems and have the AI classify them.
“Because of the breakthrough with deep learning, it’s becoming possible to make AI with performance similar to human performance,” said Kenji Suzuki, an associate professor of electrical and computer engineering at the Illinois Institute of Technology.
Using artificial intelligence to make medical diagnoses may seem like a very recent development, but the idea has been under development for several decades. Research on using AI to help healthcare professionals identify signs of disease in medical images began in earnest in the early 1980s. The Kurt Rossmann Laboratories for Radiologic Image Research at the University of Chicago acted as a key research hub at this time, attempting to train AI to identify lesions in lung images.
In 1995, the FDA issued its first approval of an artificial intelligence image-reviewing technology, the AutoPap 300 QC System. This
A pathologist would always check the slide for abnormal cells as well, meaning the AI system acted as a kind of
IDx-DR and other new AI programs share several advantages. First, AI can process an image in seconds, much faster than locating an expert and having them look at the image, and can reduce the strenuous workload of human experts.
The University of Iowa Health Care was the first hospital to use IDx-DR technology in a clinical setting. Dr. Yumi Imai, associate professor of internal medicine at the hospital, said that the AI-assisted retinal screening takes only about 10 minutes during a standard physical exam, instead of the hours it would take to travel to and complete an appointment with an ophthalmologist. “I think it’s very time-saving,” she said.
Second, the best image-reviewing AI programs now have a level of accuracy comparable to that of human experts and can be used to double-check an expert’s work, helping to prevent errors. Third, AI programs are potentially valuable tools in rural areas where people might have great difficulty commuting to a specialist.
However, image-reviewing AI programs also have significant limitations. Although AI programs can be highly effective at identifying very specific health issues, they can’t detect other problems. For example, unlike a human ophthalmologist, an AI that detects problems with retinal blood vessels will not detect cataracts during the same examination.
Aristotelis Tsirigos, an associate professor of pathology at New York University, published a study in Nature Medicine in September 2018 that showed that an AI could differentiate between two subtypes of non-small cell lung cancer. The AI was as effective as a human at this task, but it could not classify the third subtype of non-small cell lung cancer or the other two main types of lung cancer because it was not trained to do that.
“In this study, we just focused on a very narrow task that pathologists do, but pathologists do many more things,” Tsirigos said. “They don’t just make a distinction between two types [of lung cancer] … So it will take a lot of time for AI to catch up, I think.”
No matter how advanced AI programs become, they will not help many people if they are too costly. Dr. Imai said that IDx-DR would probably be too expensive for small, rural doctors’ offices, where they could have the biggest impact, but might be obtainable for group practices. An eye-scanning AI in a single-physician office in Montana will likely remain a novel concept through the near future.